Gastrointestinal Tract Histology
Overview of Gastrointestinal Tract Histology
Gastrointestinal Tract
The gastrointestinal tract (GIT) comprises the stomach, duodenum, jejunum, ileum, colon, rectum and anal canal. The GIT and oesophagus form the alimentary canal.
The Stomach
The stomach functions both as a reservoir and as a digestive organ. It empties its contents in small portions (suitable for continued digestion) into the small intestine.
Anatomically, the stomach is divided into:
- a cardiac part,
- fundus,
- body or corpus, and
- a pyloric part (pyloric antrum and pyloric canal)
Histologically, most of the layers of the wall of the stomach appear similar in its different parts. Regional differences are mainly restricted to the appearance of the gastric mucosa.
The Mucosa (epithelium, lamina propria, muscularis mucosae)
The mucosa is thrown into longitudinal folds (gastric folds or rugae), which disappear when the stomach is fully distended. A network of shallow grooves divides the mucosa into gastric areas (1-5 mm). On the mucosal surface we see small, funnel-shaped depressions (gastric pits). Almost the entire mucosa is occupied by simple, tubular gastric glands which open into the bottom of the gastric pits.
The structure and cellular composition of the surface epithelium (simple, tall columnar) does not change throughout the stomach. It contains mucus-producing cells, surface mucous cells, which form a secretory sheath (glandular epithelium). The mucus is alkaline and adheres to the epithelium. The mucus forms an ~ 1 mm thick layer, which protects the mucosa from the acidic contents of the stomach. The surface epithelium is renewed approximately every third day. The source of the new cells is the isthmus, i.e. the upper part of the neck, of the gastric glands, where cells divide and then migrate towards the surface epithelium and differentiate into mature epithelial cells.
In contrast to the surface epithelium, cellular composition and function of the gastric glands are specialized in the different parts of the stomach.

Cardiac glands
Cardiac glands are heavily branched tubular glands (similar to the cardiac glands of the esophagus), which contain mainly mucus-producing cells. A few of the secretory cells characteristic for the principal glands (see below) may be present.
Principal (or corpus-fundic) glands
Each glandular tubule (oriented more or less perpendicular to the surface of the epithelium) consists of three parts: a deep body, an intermediary neck and an upper isthmus. In principal glands we find four cell types: chief cells, parietal cells, mucous neck cells and endocrine cells.
Chief cells (or zymogenic cells)
are the most numerous of the four types. They occur primarily in the body of the glands. They produce pepsinogen, which is a precursor of the proteolytic enzyme pepsin.
The pH optimum of of pepsin is about 2. This enzyme is able to break down collagen.
Parietal cells (or oxyntic cells)
occur most frequently in the neck of the glands, where they reach the lumen of the gland. They are situated deeper, between and below chief cells, in lower parts of the gland. Parietal cells secrete the hydrochloric acid of the gastric juice. Aside from activating the pepsinogen the hydrochloric acid also effectively sterilizes the contents of the stomach.
Note that so far only one type of bacteria has found which can live happily in the stomach -Helicobacter pylori. Unfortunately these bacteria are involved in the pathogenesis of gastritis and gastric ulcers.Parietal cell also secrete intrinsic factor, which is necessary for the resorption of vitamin B12.
Vitamin B12 is a cofactor of enzymes which synthesise tetrahydrofolic acid, which, in turn, is needed for the synthesis of DNA components. An impairment of DNA synthesis will affect rapidly dividing cell populations, among them the haematopoietic cells of the bone marrow, which may result in pernicious anemia. This condition may result from a destruction of the gastric mucosa by e.g. autoimmune gastritis or the resection of large parts of the lower ileum, which is the main site of vitamin B12 absorption, or of the stomach.
Mucous neck cells
are found between the parietal cells in the neck of the gland. They are difficult to distinguish from chief cells in plain H&E stained section.
Endocrine cells
Endocrine cells are scattered, usually solitary, throughout the epithelium of the gastrointestinal tract. They are part of the gastro-entero-pancreatic (GEP) endocrine system. The best characterized endocrine cells in the gastric mucosa are gastrin-producing cells (G cells) and somatostatin-producing cells (D cells). G cells are most frequent in the middle third of the glands. They stimulate the secretion of acid and pepsinogen. G cell function is stimulated by nervous input, the distension of the stomach or secretagogues. D cells are found mainly in glands of the pyloric antrum. They inhibit G cells and thereby acid production. D cell function is stimulated by acid in the lumen of the stomach and duodenum.
Other types of endocrine cells encompass VIP-producing cells (or D1 cells; vasoactive intestinal peptide) and serotonin-containing cells (enterochromaffin cells). Endocrine cells in the gastrointestinal tract are alternatively named APUD-cells: amine precursor uptake and decarboxylation cells.
Pyloric glands
Pyloric glands are more coiled than principal glands, and they may be branched. Endocrine cells, in particular gastrin-producing cells, are more frequent than in principal glands. A few parietal cells may be present but chief cells are usually absent.
The lamina propria is formed by a very cell-rich loose connective tissue (fibroblasts, lymphocytes, plasma cells, macrophages, eosinophilic leukocytes and mast cells). The muscularis mucosae of the stomach contains both circular and longitudinal layers of muscle cells. Its organization is somewhat variable depending on the location in the stomach.
Large blood vessels, lymph vessels and nerves are located in the submucosa which consists of loose connective tissue.
Note that the muscularis externa consists of three layers of muscles: an inner oblique layer, a middle circular layer and an outer longitudinal layer.
Small Intestine
The small intestine is divided into duodenum (25-30 cm), jejunum (about first two-fifths of the rest) and ileum. The three segments merge imperceptibly and have the same basic histological organization.

The Mucosa
The mucosa of the small intestine has various structural features which considerably increase the luminal surface area and consequently support the main function of the small intestine – the absorption of the degraded components of the food.
Plicae circulares (of Kerkering) are macroscopically visible, crescent-shaped folds of the mucosa and submucosa. Plicae circulares extend around one-half to two-thirds of the circumference of the lumen of the small intestine.
Plicae circulares
- are permanent structures, i.e. their presence does not depend on the state of distension of the small intestine.
- are absent from the first few centimetres of the duodenum and the distal part of the ileum.
- Are particularly well developed in the jejunum.
- increase the surface area of the mucosa by a factor of ~ three.
The entire intestinal mucosa forms intestinal villi (about one mm long), which increase the surface area by a factor of ~ ten. The surface of the villi is formed by a simple columnar epithelium. Each absorptive cell or enterocyte of the epithelium forms numerous microvilli (1 µm long and about 0.1 µm wide). Microvilli increase the surface area by a factor of ~ 20.
Between the intestinal villi we see the openings of simple tubular glands, the crypts of Lieberkühn. They extend through the lamina propria down to the muscularis mucosae. Undifferentiated cells close to the bottom of the crypts regenerate the epithelium (epithelial cell turnover time is less than one week). Other epithelial cells in the crypts correspond largely to those in the epithelium of the intestinal villi. One exception are Paneth cells which are located at the bottom of the crypts. They release a number of antibacterial substances, among them lysozyme, and are thought to be involved in the control of infections.
One function of the crypts of Lieberkühn is the secretion of “intestinal juice” (about 2 liter/day), which in its composition closely resembles extracellular fluid and which is rapidly reabsorbed. The only enzymes which can be demonstrated in the intestinal juice are enteropeptidase (or enterokinase), which activates the pancreatic enzyme trypsin, and small amounts of amylase. In addition to enterocytes, the epithelium is composed of mucus-secreting goblet cells and endocrine cells.
In addition to gastrin- and somatostatin-producing cells, we also find endocrine cells secreting cholecystokinin and secretin. Cholecystokinin stimulates the secretion of digestive enzymes in the pancreas and the contraction of the gall bladder. Secretin stimulates the pancreas to release “pancreatic juice”, which is rich in bicarbonate ions. Secretin also amplifies the effects of cholecystokinin.

The lamina propria is, similar to the lamina propria of the stomach, unusually cell rich. Lymphocytes often invade the epithelium or form solitary lymphoid nodules in the lamina propria. Lymph nodules may form longitudinal aggregations of 30-50 nodules in the lamina propria of the ileum. These large aggregations are called Peyer’s patches.
The muscularis mucosae has two layers and extends into the intestinal villi, where the smooth muscle cells form a longitudinal bundle in the centre of the villi.
The Submucosa
The submucosa contains glands only in the duodenum. Submucosal glands of the duodenum are also called Brunner’s glands. Their secretion is mucous and slightly alkaline due to bicarbonate ions (pH 7-8). The amount of bicarbonate is however too low to neutralize the acidic contents of the duodenal lumen. Instead, the secretion of Brunner’s glands protects the duodenal mucosa – similar to the mucus which protects the gastric mucosa.
Large Intestine
The large intestine constitutes the terminal part of the digestive system. It is divided into three main sections: cecum including the appendix, colon, and rectum with the anal canal. The primary function of the large intestine is the reabsorption of water and inorganic salts. The only secretion of any importance is mucus, which acts as a lubricant during the transport of the intestinal contents.
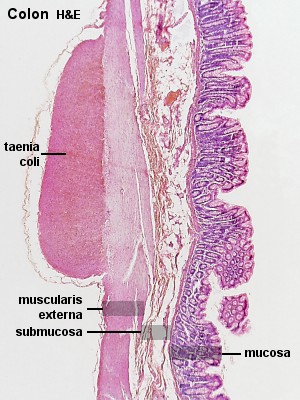
The surface of the mucosa is relatively smooth as there are no plicae circulares or intestinal villi. Crypts of Lieberkühn are present and usually longer and straighter than those of the small intestine. Goblet cells account for more of the epithelial cells than in the small intestine.
There is only little lamina propria squeezed between the glands. The muscularis mucosae again forms two layers.Considerable amounts of fat may be found in the submucosa.
The appearance of the muscularis externa is different from that of the small intestine. The inner circular layer of muscle forms the usual sheath around the large intestine, but the outer longitudinal muscle layer forms three flattened strands, the taenia coli. Only a thin layer of longitudinal muscle surrounds the inner circular muscle layer between the taenia coli .
The adventitia forms small pouches (appendices epiploicae) filled with fatty tissue along the large intestine.
Specialized Sections of the Large Intestine
The vermiform appendix

is a small blind-ending diverticulum from the cecum. The most important features of the appendix is the thickening of its wall, which is mainly due to large accumulations of lymphoid tissue in the lamina propria and submucosa. Intestinal villi are usually absent, and crypts do not occur as frequently as in the colon. There is often fatty tissue in the submucosa. The muscularis externa is thinner than in the remainder of the large intestine and, the outer, longitudinal smooth muscle layer of the muscularis externa does not aggregate into taenia coli.
An extreme proliferation of lymphocytes (lymphoid hyperplasia) as a consequence of bacterial or viral stimulation may lead to the obstruction of the lumen of the appendix and thereby cause appendicitis, but this is only one of many possible causes.
The anal canal
is the 2.5-4 cm long terminal part of the digestive tract. The mucosa has a characteristic surface relief of 5-10 longitudinal folds, the anal columns.
Each column contains a terminal branch of the superior rectal artery and vein.
Small mucosal folds between the anal columns (anal valves) form the pectinate line. This line defines sections of the anal canal with different arterial and nerve supplies, different venous and lymphatic drainages and different embryological origins. Crypts disappear below the pectinate line and the epithelium changes from the tall, columnar type seen in other parts of the large intestine to a stratified squamous epithelium. The muscularis externa gradually becomes thicker and forms the involuntary internal anal sphincter.
Junctions
Junctions between the major parts of the alimentary canal share a rapid transition from tissues characteristic of one part to those characteristic for the next part, e.g. the transition from the stratified squamous epithelium of the oesophagus to the glandular epithelium of the stomach. Many junctions are in addition accompanied by morphological specializations, e.g. the pylorus at the gastro-duodenal junctions or the ileo-caecal valve at the ileo-caecal junction.
Compared with these rapid changes, “junctions” between parts of the small intestine are very gradual morphological transitions.